Pneumatosis intestinalis with delayed onset small bowel perforation: a case report
Article information
Abstract
Pneumatosis intestinalis (PI) is an uncommon abdominal pathology, and its global incidence is 0.03%. The clinical course of PI ranges from benign to life-threatening and delayed onset of complicated small bowel perforation is very rare. An 84-year-old male presented with sudden-onset, postprandial, epigastric pain. Abdominal computed tomography scan at the emergency department revealed PI with diffuse right colon dilation and hepatic portal venous gases. He did not present critical signs and responded well to conservative management after hospitalization. However, 19 days later, he developed sudden, diffuse, abdominal pain, which was caused by delayed small bowel perforation. He underwent resection of the small intestine by a general surgeon, and admitted at intensive care unit for postoperative treatments, but died 3 months after admission. Delayed onset of complications such as perforated peritonitis is rare but life-threatening in PI patients, and therefore, they should be monitored carefully.
INTRODUCTION
Pneumatosis intestinalis (PI) is an uncommon abdominal pathology worldwide which was first reported in 1754 [1,2]. It characterized by the presence of abnormal gaseous formations in the wall of the gastrointestinal tract (GIT) [3]. Although the leading cause of PI is unknown, about 15% of the cases are idiopathic and called pneumatosis cystoides intestinalis (PCI), and other cases are a consequence of various diseases such as ischemic bowel disease, connective tissue disease, several medications, and chronic obstructive pulmonary disease (COPD) [2,4]. PI could be accompanied by several medical problems such as portal venous air, mesenteric ischemia, and pneumoperitoneum [4,5]. Of these, pneumoperitoneum, which may or may not be associated with intestinal perforation, could be occur, especially those associated with perforated peritonitis is an uncommon complication in PI patients [6]. Here, we report a case of a patient with acute abdominal pain caused by PI and delayed onset small bowel perforation.
CASE REPORT
An 84-year-old male visited the emergency department (ED) with sudden-onset, postprandial, and epigastric pain. He had dinner 2 hours prior to arrival at the hospital, and the symptom started 1 hour after dinner. He had a history of ischemic heart disease, COPD, chronic atrophic gastritis with intestinal metaplasia, and rheumatoid arthritis. In addition, he had undergone cholecystectomy and surgery for right inguinal hernia. He did not smoke or consume alcohol. His initial vital signs included blood pressure of 110/80 mmHg, heart rate of 70 beats/min, respiratory rate of 20 breaths/min, and normal body temperature. He had nausea and diffuse epigastric pain, and direct tenderness but no rebound tenderness or board-like rigidity was detected on abdominal physical examination. Initial laboratory results were as follows: white blood cell count 10,290/μL, hemoglobin 9.1 g/dL, aspartate aminotransferase 20 IU/L, alanine aminotransferase 10 IU/L, serum amylase 266 IU/L, serum lipase 6 IU/L, total bilirubin 0.72 mg/dL, direct bilirubin 0.16 mg/dL, blood urea nitrogen 35 mg/dL, serum creatinine 0.81 mg/dL, blood lactate level 2.3 mmol/L, and C-reactive protein 0.175 mg/dL. Simple X-ray scans at the ED showed no specific, abnormal pathologic findings (Fig. 1). However, the abdominal computed tomography (CT) scan showed gas formation within the intestinal wall with diffuse bowel dilation in the right ascending colon and hepatic portal venous gas formations, and the patient diagnosed with PI (Fig. 2). There were no specific abnormal pathologic lesions in the small bowel.

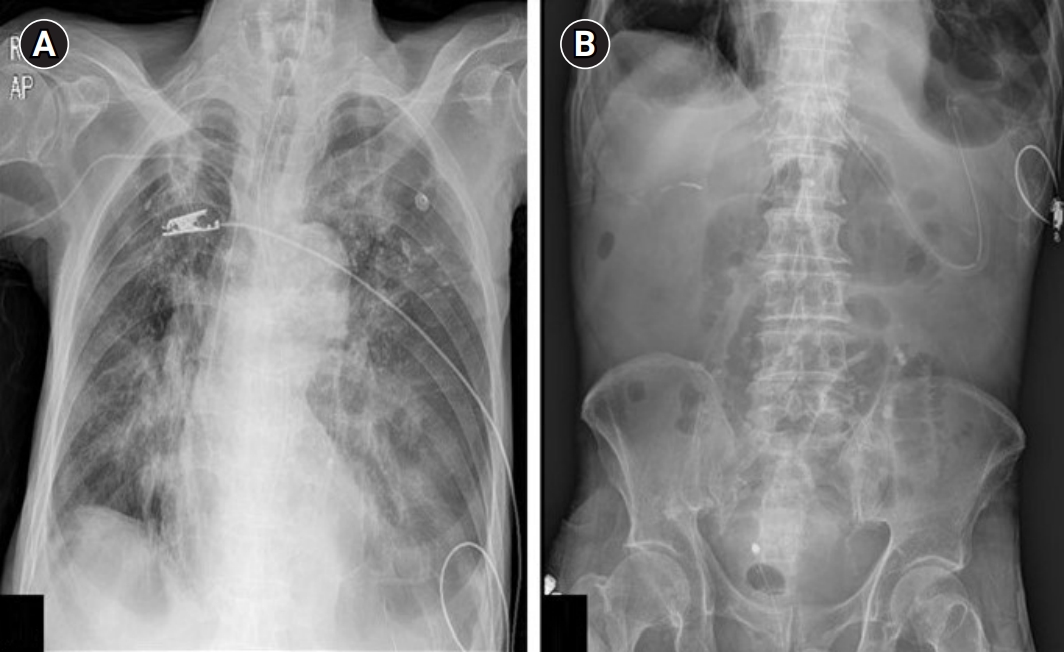
Simple X-ray scans at the emergency room showed emphysematous lung and old pulmonary tuberculosis scar, but there were no specific acute pathological findings such as pneumoperitoneum. (A) Erect posteroanterior chest radiograph and (B) simple abdomen supine.

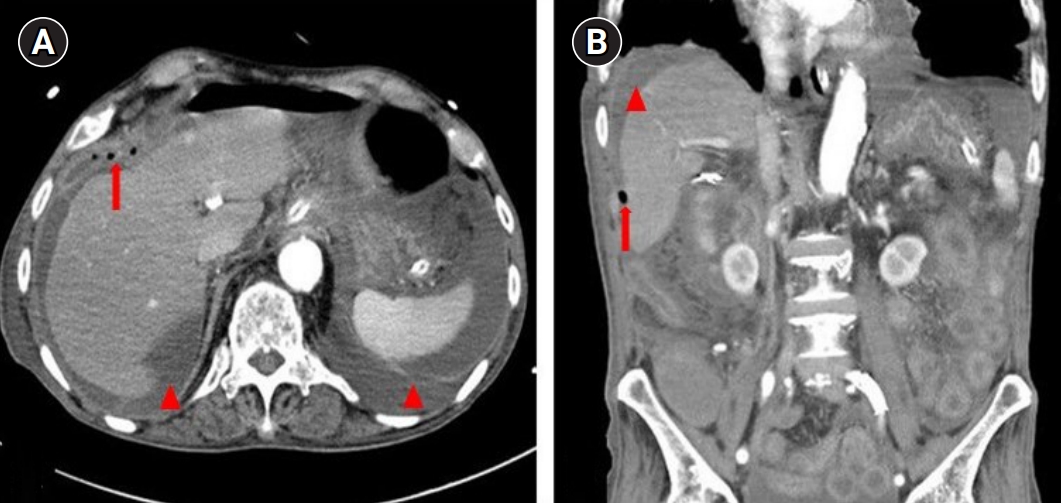
Abdominal computed tomography scans at the emergency department. Arrows are indicated the pneumatosis intestinalis with diffuse bowel dilation in the right colon, and arrowheads are indicated hepatic portal venous gases. (A, B) Transverse view and (C, D) coronal view.
He was hospitalized in the general surgery department for conservative treatment including fasting, fluid and electrolyte managements, and intravenous (IV) antibiotics because his vital signs were stable with no sign of critical complication. Oxygen inhalation therapy was also administered. His general condition was stably maintained for 18 days since admission, but he suddenly complained of diffuse abdominal pain on the 19th day of hospitalization. His follow-up simple X-ray scan showed no abnormal pathologic finding such as intra-abdominal free air (Fig. 3). However, abdominal CT scan showed several, newly developed focal air shadows and a large number of ascites around the liver and spleen (Fig. 4). He was diagnosed with peritonitis caused by small bowel perforation and underwent resection of the small intestine by a general surgeon. However, he progressed to sepsis and died 3 months later despite the intensive postoperative care and aggressive critical management including mechanical ventilation support, IV adrenalin and antibiotics.
Simple X-ray scans 19 days after hospitalization did not show valuable intra-abdominal free air. (A) Supine anteroposterior chest radiograph and (B) simple abdomen supine.
DISCUSSION
PI is a pathological condition characterized by gaseous formations within the wall of the GIT, and its global incidence is 0.03% [2,7]. In addition, it is called PI coli, pneumatosis cystoides intestinorum, PCI, and PCI hominis [8]. Most cases occur in the colon (46%), small bowel (27%), and rarely both (7%) [2]. In this case, the initial radiological identification of PI was made in the colon, but perforation occurred in the small intestine.
PI is classified as primary and secondary but it is often difficult to differentiate between the two types [3]. The pathophysiology of PI is unclear but there are two potential theories for secondary PI. In the mechanical theory, predisposing conditions such as intestinal obstruction causing intestinal wall breaks that increase the intra-luminal pressure and lead to forced invasion of gases. In addition, COPD can cause pneumomediastinum by alveolar rupture which could lead to gaseous formations that travel from the aorta to the mesenteric vessels and bowel wall. In the bacterial theory, overgrowth of gas-forming bacteria in the enteric lumen produces massive quantities of hydrogen gas, increases the luminal pressure, and forces entrapment of the gas in the intestinal wall. In addition, bacterial invasion through the enteric mucosal area leads to gas formations in the intestinal wall [6,9]. In this case, we suspected that the patient had secondary PI because of COPD [8].
The most useful and frequently used diagnostic method for detecting PI is the abdominal CT scan [5]. Diagnostic laparoscopy could be helpful in the identification of intestinal perforation, bowel ischemia, or necrosis when clinically suspected [9]. Colonoscopy could be useful to distinguish between PI and other pathogenic lesions of the colon [6].
The clinical course of PI varies from asymptomatic to life-threatening acute abdominal pathologies such as mesenteric ischemia, intestinal obstruction, enteritis, colitis, trauma, organ transplantation, or collagen vascular disease [2,5]. In addition, the management of PI is challenging, and includes from conservative management such as parenteral nutrition, fluid and electrolyte support, IV antibiotics, GI decompression and rest, to even emergency operation [3,6,9]. Inhalation oxygen could be consider for alleviate symptoms because its toxic effect to intestinal anaerobic bacteria [3]. Generally, it managed by non-surgically but critical complications require surgical intervention [4,6,9]. Factors associated with surgical intervention included hypotension, suspected need for surgery on physical examination, elevation of blood lactate >2 mmol/L, serum bicarbonate <20 mmol/L, leukocytosis >12 K/μL, age >60 years, and a sharp increase in serum creatinine, ascites, portal vein gases, or bowel dilatation [2,3].
PI is not a clinical diagnosis but a radiological sign and it can be idiopathic or associated with various etiologies [8]. Since the progress varies from benign to fatal, clinical conditions and laboratory results are important in the management and treatment of PI [3,5,6]. We suspected that PI in our patient was related to COPD which is generally benign [5]. In addition, pneumoperitoneum was not seen in the ED. Although his age was over 60 years and an abdominal CT scan showed portal venous gases, he did not present any other critical sign such as an acute abdominal sign on physical examination or serious laboratory findings. Thus, the patient was treated by conservative management [4,6,8]. However, he developed critical complications 19 days after hospitalization and despite our best efforts the patient died.
True intestinal perforation is uncommon but life-threatening in a PI patient. In addition, timely detection of intestinal perforation is difficult but necessary for treatment of PI patient [5,6,10]. The occurrence of delayed onset perforation is very rare but it could be. Therefore, physicians should take care that this life-threatening complication could arise over time even in PI patients who are stable and respond well to conservative treatment.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
AUTHORS’ CONTRIBUTIONS
Conceptualization: SBL, JHK; Data curation: JHK; Formal analysis: JHK; Investigation: SBL, JHK; Methodology: JHK; Project administration:all authors; Resources: SBL, JHK; Software: KJH; Supervision: SBL; Validation: SBL, JHK; Visualization: SDS, JHP; Writing–original draft: JHK; Writing–review & editing: all authors.